For all parents, it can be very worrying when your baby is unwell, even if they are suffering from something which turns out to be quite minor.
Talk to your GP or health visiting team if something doesn’t seem quite right to you – they are there to support you.
The minor ailment scheme
You do not always have to see your GP for minor ailments. Some pharmacies run what’s known as a minor ailment scheme for specific ailments, such as coughs and colds and diarrhoea and vomiting.
When pharmacies provide medicines as part of a minor ailment scheme, you get the medicines on the NHS. You will not pay a prescription charge for children under 16.
Not all pharmacies offer a minor ailment scheme, and the ailments covered by the scheme vary from area to area.
Scroll through the different ailments and illnesses below and click the titles for more information and support.
Vomiting/sickness and diarrhoea
The most common cause of diarrhoea and vomiting in babies and young children is a tummy bug, which usually only last a couple of days.
You can usually treat your child at home for sickness and diarrhoea. The most important thing is to give them lots of fluids to drink to avoid dehydration.
Sickness and diarrhoea bugs are caught easily, so encourage everyone in the family to be extra vigilant about handwashing.
Keep breastfeeding them or giving them formula feeds as normal so that they stay hydrated. If they are vomiting, offer smaller volumes of milk or frequent breastfeeds.
Don’t dilute formula milk. Remember to make formula milk to the strength as directed on the instructions. Read more about making up feeds here.
If your baby or child is having solid food, don’t worry if they don’t want to eat much. Just make sure you regularly offer water for them to drink.
If your baby/child has a temperature, you may want to give infant paracetamol. Don’t give paracetamol to a child under the age of two months without medical advice.
Look out for signs of dehydration, which include:
- fewer wet nappies
- sleepiness
- a sunken fontanelle – the soft spot on the top of the baby’s head
-
If your child has any of these signs of dehydration, your baby continues to be sick for more than 48 hours, or you’re worried that something more serious is going on, contact your GP.
If your baby is less than 12 months old and has vomiting/diarrhoea, speak to your GP or health visiting team.
If they seem floppy or less responsive, seem to have a stiff neck or a rash, call 999 for an ambulance or go to your nearest A&E department immediately.
Coughs, colds and earache
- a blocked or runny nose
- a sore throat
- headaches
- muscle aches
- coughs
- sneezing
- a raised temperature
Usually these don’t last longer than a week, and you there are lots of things you can do at home to help their symptoms.
For babies over 6 months, offer water or very diluted fruit squash, making sure they drink plenty and stay hydrated.
If your child has a cough and is over the age of one, they can try drinking a warm drink of lemon and honey. Do not give your child honey until they’re over one year old.
To make lemon with honey at home, you need to:
- Squeeze half a lemon into a mug of boiled water
- Add one to two teaspoons of honey
- Do not drink while boiling hot. Allow the drink to cool, but drink while still warm. Do not give drinks to small children whilst they are hot. Always check the temperature beforehand to avoid the risk of burns and scalds
If your child has had a cough that’s lasted longer than 3 weeks, see your GP.
If they have a temperature or are in a lot of discomfort, you may want to give them some children’s paracetamol or ibuprofen; always follow the instructions on the packaging.
Saline nasal drops can also help a stuffy nose; ask your GP, Pharmacist or health visiting team about them.
Don’t use plug in or inhaled decongestants for babies under 3 months old. Children under the age of six should not have over the counter cough and cold remedies unless advised to by a GP or pharmacist.
If your baby has a barking cough and is making a harsh sound when they breathe in, they may be suffering from croup. These symptoms may go hand-in-hand with a runny nose, sore throat and high temperature. Get an appointment with your GP who will check your baby over and advice on treatment.
If the symptoms are severe and your child is finding it hard to breathe, take them to accident and emergency (A&E) straightaway.
![]()
Ear infections
- your baby’s ear looking a bit red
- your baby pulling or rubbing their ear
- irritability and restlessness
- difficulty feeding
- discharge from the ear
-
Whether they have a temperature or not, you can treat the pain of ear ache with children’s paracetamol or ibuprofen, making sure you follow the instructions on the packaging.
After an ear infection, you may find your child’s hearing is affected for a few weeks. If the problem carries on, talk to your GP.
When children suffer with lots of ear infections, it can sometimes lead to the build-up of sticky fluid in the middle ear, which can affect their hearing. This is known as ‘glue ear’. Your GP will advise you about treatment.
Breathing and wheezing
It might be that they have taken in their milk too quickly, which is causing them to cough or splutter a bit, so check their feeding position and try to slow things down. It may help to hold them upright.
If your baby does have a cold or mild cough, keep an eye on them and talk to your health visiting team if you’re worried.
Bronchiolitis is a common respiratory infection that can affect children under the age of two. Most cases are mild and will resolve within 2-3 weeks. The symptoms of bronchiolitis can be similar to those of a common cold. Further symptoms can also develop, including:
- A raised temperature
- A dry and persistent cough
- Problems feeding
- Wheezing
-
You should seek further advice from your GP if you are concerned about your child, if they have a persistent high temperature, are not feeding normally and taking less than half of their usual amounts of feeds, or they have not had a wet nappy for 12 hours or more.
Call 999 or take them straight to A&E if their breathing is really laboured (flaring nostrils or the spaces between the ribs goes in when breathing) or if they look very pale or slightly blueish.
Rashes
Go to A&E or call 999 if your child has a rash and they:
- have a stiff neck
- are bothered by light
- seem confused
- are shaking uncontrollably
- have a fever you can’t control
- have unusually cold hands and feet
- (have a rash) that doesn’t fade when you press a glass against it
-
Slapped cheek syndrome

This presents as a bright red rash on both cheeks. Your child can feel unwell, have a fever and the rash might spread to other areas of the body.
This should get better within a week, but speak to a GP if you’re concerned. You can use children’s paracetamol to help with a fever, never use an adult brand or dose of paracetamol.
Hand, foot and mouth disease

This can cause blisters on the hands and feet, it might also cause ulcers on the tongue and be accompanied with a fever and cold.
This should get better within a week, but speak to a GP if you’re concerned. You can use children’s paracetamol to help with a fever, never use an adult brand or dose of paracetamol.
Scarlet fever

Causes a blotchy rash that is pink/red in colour, it will look like sunburn and feel rough like sandpaper. It might be accompanied by a swollen tongue, sore throat, headache and fever. Scarlet fever will need to be treated with antibiotics, so speak to a GP as soon as possible.
Measles

Grey spots inside the cheeks and sore eyes that are sensitive to light and a fever are all early signs of measles. A red/brown coloured rash will appear on the head or neck and spread across the body. Speak to a GP if you suspect your child has measles.
Heat rash

Small itchy red spots caused by heat and sweat are known as heat rash. This does not need treatment.
Eczema


Dry, cracked, itchy and red skin might be eczema. You should speak to your GP if you suspect your child might have eczema.
Newborn acne (erythema toxicum neonatorum)

Newborn acne is a common skin rash affecting healthy newborn babies. It is not serious, does not cause the baby any harm and clears up without any treatment. Don’t attempt to pop or squeeze the pimples. Doing so may cause an infection.
The NHS website has a really useful visual guide to many other different rashes you may come across.
Nappy rash
Nappy rash can be very sore, but it is fairly easy to treat.
When nappy rash develops, the skin around the baby’s nappy area becomes inflamed, hot to the touch and, if the rash persists, small blisters can appear.
Nappy rash happens when the baby’s skin has contact over a period of time with wee or poo in the nappy, regardless if you use re-usable nappies or disposable ones. The skin can also become sore when the nappy rubs against it.
Nappy rash doesn’t always happen because a soiled nappy has been left on too long – it may be that your baby has particularly sensitive skin.
Nappy rash is also more likely when your baby:
- Is suffering from diarrhoea – the substances in poo that irritate the skin are more concentrated in runny poo
- Has had an allergic reaction, for example to perfumed baby wipes, soap, detergent or a particular brand of nappy. Nappy rash can also be caused by lactose intolerance or a food allergy. If you think this is the cause, talk to your GP
- Has been given antibiotics. Sometimes nappy rash is caused by a fungal infection called thrush, and taking antibiotics makes you more likely to suffer from thrush
-
Preventing and treating nappy rash
- Make sure you change wet or dirty nappies as soon as possible.
- Clean the whole area thoroughly using water or fragrance-free baby wipes.
- If your baby is particularly prone to nappy rash, choose a brand of nappy that is super absorbent
- Give your baby regular baths then dry their skin gently by patting with a towel rather than rubbing.
- Give your baby some time to lie on a towel or changing mat with their nappy off so that fresh air gets to the skin.
- Avoid perfumed bubble bath and soap
- Apply a barrier cream to your baby’s bottom
-
Mild cases of nappy rash should clear up after two to three days. If the rash is severe and is causing your baby discomfort, your GP or health visiting team may prescribe, or advise you use a special cream to soothe and treat it, as well as a barrier cream to prevent further infection.
Cradle cap
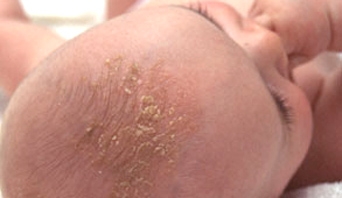
Young babies often develop scaly yellow or brown patches on their scalp, and this is known as ‘cradle cap’. Sometimes the scales flake off and the skin can look a bit red underneath.
Cradle cap is common and doesn’t cause any itching or discomfort for your baby. You should avoid picking at the scales though as this could cause an infection.
There are some things you can do to reduce the scaly build-up:
- Brush your baby’s scalp using a soft baby hair brush, even if your baby doesn’t have a lot of hair, at least twice daily
- Use a baby shampoo to wash your baby’s scalp regularly and then brush with a soft baby brush to loosen the flakes
- If these treatments don’t work, special shampoos are available from the pharmacy. Your pharmacist will be able to advise you about which ones are appropriate. Don’t use shampoo if your baby has eczema.
-
If the cradle cap starts to look red and sore, consult your GP, as it may have become infected.
Chickenpox

Chickenpox is common, especially in children. It starts with red itchy spots, these can appear anywhere on the body and can spread or just stay in one area. These spots blister and fill with fluid before they scab over, new spots can appear whilst others are blistering. Your child may also experience aches and pains or a high temperature.
Chickenpox is highly contagious, it can be caught by being in the same room as someone with it, so your child will need to stay away from school or nursery until all spots have crusted over. Chickenpox can be caught more than once, but this is unlikely. It can be treated from home and most people won’t need to speak to a GP.
Tips for treating chickenpox from home:
- Speak to a pharmacist about cooling creams or gels available over the counter
- Bathe your child in cool water and pat their skin dry (do not rub)
- Give your child plenty of fluid to avoid dehydration
- Put socks on your child’s hands at night to avoid them scratching
-
DO NOT:
- use ibuprofen unless advised to do so by a doctor, as it may cause serious skin infections
- give aspirin to children under 16
- mix with pregnant women, newborn babies and people with a weakened immune system, as chickenpox can be dangerous for them
-
Speak to a GP or 111 if:
- Your newborn baby has chickenpox
- You’re pregnant, have never had chickenpox before and have come into contact with someone with chickenpox
- You or your child have a weakened immune system and have come into contact with someone with chickenpox
- You’re concerned about their condition worsening
-
Head lice
If you find live head lice in your child’s hair, they do not need to see a GP or have time off school. You should check everyone in the house, including adults, and treat everyone who has head lice on the same day.
Before buying any medicated lotions or sprays, try wet combing the affected hair first. You can do this by using a detection comb to comb hair thoroughly, from the roots to the ends, after it has been washed with shampoo and conditioner. Longer hair will take more time to comb. You should wet comb on days 1, 5, 9 and 13 to get rid of any newly hatched head lice. Check that everyone’s hair is free of lice on day 17.
If there are still head lice after 17 days, speak to a pharmacist about medicated sprays or lotions designed to kill head lice. There are treatment methods that are not recommended as they are unlikely to be effective, these include:
- products containing permethrin
- head lice “repellents”
- electric combs for head lice
- tree and plant oil treatments, such as tea tree, eucalyptus and lavender oil
-
Head lice cannot be prevented, do not try to use sprays or treatments to prevent lice as they can irritate the scalp and will not work.
Threadworms
The worms look like small pieces of white thread, you might be able to see them in your child’s poo or around their bottom. Your child might also experience itching or irritability, especially during the night.
Threadworms lay eggs around the anus which can cause itching, the eggs can then be transferred onto hands when the area is scratched and pass onto any surface that is touched – the worms are spread when their eggs are ingested. So it’s important to encourage children to wash their hands regularly and thoroughly (link to further info about hand washing). You should also wash your hands and scrub underneath your fingernails after changing nappies.
If anyone in your household has threadworms, there is no need to stay away from school, work or nursery. But make sure you speak to a pharmacist about treatment. Everyone in your household should receive treatment, even if they show no symptoms.
Speak to your GP if you’re pregnant, breastfeeding or have any children under 2.
Medicine will kill the threadworms but not their eggs, these will survive for up to two weeks outside of the body and can infect members of your household again. Disinfect surfaces, wash hands regularly and shower daily to prevent re-infection.
Useful links
- NHS website – Diarrhoea and vomiting
- NHS website – Coughs, colds and ear infections in children
- NHS website – Nappy rash
- NHS website – Health
- Leicester’s Hospitals – A parents guide to self care at home for children aged 0-9
- The Lullaby Trust- Infection and illness
